
The liver is a remarkably resilient organ. It absorbs stress quietly, adapts silently, and continues to function, even when damage has already begun. This is precisely why liver diseases are often detected late. Sometimes, liver care doctors come across patients whose blood tests look normal, but their liver may require medical attention.
We speak to Dr Sandeep Satsangi, Lead Consultant – Hepatology and Transplant Hepatology, Manipal Hospital, Old Airport Road, to understand what common liver-related diseases are and what signs to keep an eye out for.
In India today, the most common causes of chronic liver disease are no longer rare or exotic. At the top of the list is fatty liver, a lifestyle-related liver disease, now known as metabolic dysfunction–associated steatotic liver disease. Alcohol-related liver disease follows closely. Other important causes include chronic viral hepatitis (especially hepatitis B and C), autoimmune liver conditions where the body attacks its own liver, and certain inherited metabolic disorders. All of these lead to liver inflammation, but often without warning signs.
Take fatty liver disease as an example. Most people feel perfectly fine in the early stages. The real clues lie in risk factors: excess abdominal weight, pre-diabetes or diabetes, high blood pressure, and abnormal cholesterol levels. A waistline above 90 cm in men or 80 cm in women, rising blood sugars, or low “good” cholesterol are not just metabolic issues but warnings that the liver is under strain.

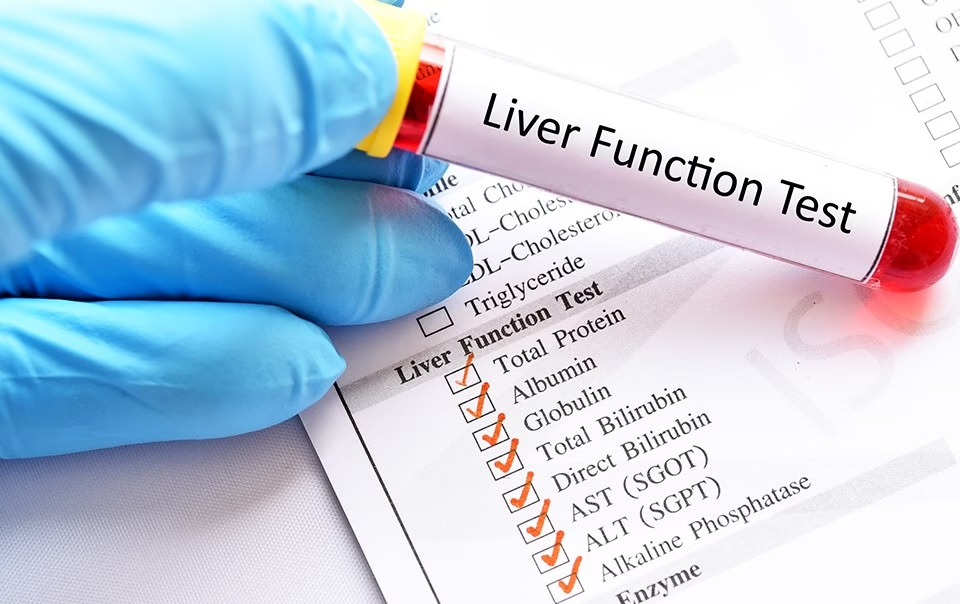
Alcohol-related liver disease behaves similarly. Even with significant alcohol intake, patients may have no symptoms, and routine liver function tests can remain within normal limits for years. Bilirubin, enzymes, albumin, and clotting markers may all look reassuring while silent damage progresses underneath. This is where many people are misled.
A normal liver function test does not always mean a healthy liver. It simply means the liver is still coping. The key, therefore, is not symptoms alone, and not blood reports alone, but risk awareness. When risk factors are present, further evaluation is essential. An ultrasound can detect fat accumulation, and specialised tests like FibroScan can identify early fibrosis. The encouraging news is that at this stage, liver damage can often be reversed with timely lifestyle changes, risk-factor control, and appropriate treatment.
The same principle applies to hepatitis B and C. Patients may feel well and see normal reports, yet fibrosis can quietly advance, increasing the future risk of cirrhosis or liver cancer. The liver rarely cries for help early. We must learn to listen before it does.






